
Caesarean birth: a global picture
19 April 2022

The picture of caesarean birth looks very different across the world. Using Chad, the UK and Brazil as case studies, we consider how both culture and health resourcing have shaped the picture of caesarean birth we see today.
A caesarean birth, also known as a C-section, is an operation to deliver a baby through a cut in the lower abdomen. A caesarean may be planned by the mother and her healthcare provider, or may be the result of an obstetric emergency; for example, where the baby is breech (lying bottom or feet first) or labour is not progressing.
A caesarean can be life-saving if a mother or her baby are experiencing complications, but can carry unnecessary risks in both the immediate and long term when it is not medically required. For example, caesareans are associated with a three- to sixfold increased risk of severe post-birth complications vs. vaginal delivery, and children born via caesarean are more likely to develop conditions such as asthma and obesity later in life.
Since 1985, the international healthcare community has agreed that the optimal caesarean rate is between 10% and 15%. However, caesarean rates are increasing, suggesting that those who would be able to deliver vaginally without severe complications are undergoing the procedure.
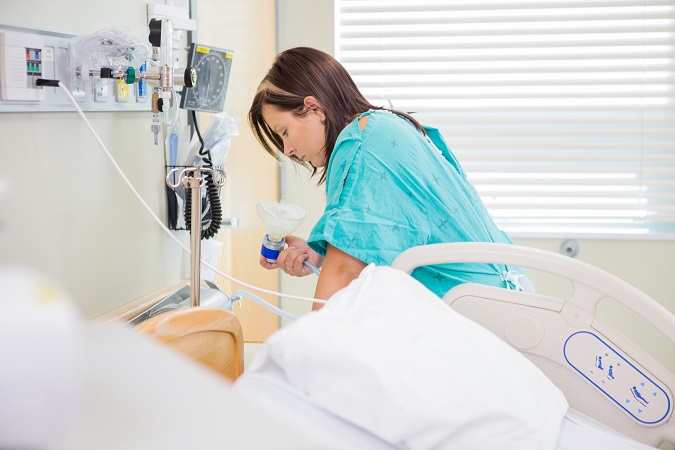
For many women, the hospital is not an ideal birthing environment: bright lights, loud noises and shift changes for hospital staff are stressors.
How do caesarean rates differ around the world?
Case study 1: Chad
Low-income countries such as Chad have little funding available for health, including maternity care. Although Chad’s government has invested heavily in healthcare infrastructure across the country, hospitals face significant staff shortages; in 2009, only 16% of women received professional support while giving birth. It is therefore unsurprising that Chad has one of the lowest rates of caesarean births in the world, at 1.4%.
Maternal mortality (death from complications during pregnancy or birth) is also a serious problem, with 1,140 out of every 100,000 women in Chad dying in childbirth in 2017. Low caesarean rates are by no means the sole influence of this incredibly high figure, but given Chad’s rate of caesarean births falls well below the optimal range, it is possible that many women die as a consequence of poor caesarean provision.
Case study 2: Brazil
In Brazil, we see a very different picture. This middle-income country has one of the highest caesarean rates in the world – 55.9% of deliveries were by caesarean in 2018. In Brazil, the risk of postpartum maternal death is almost three times higher after a caesarean birth than a vaginal birth, making caesareans a significant risk factor. Maternal mortality is also much lower than in Chad – but still not optimal – at 60 per 100,000 live births as of 2017.
Given these alarming statistics, we must call into question why caesarean rates are so high in the first place. A number of factors contribute to this; for example, healthcare is free at point of use in Brazil and doctors are paid per service provided, not by hours worked. As caesareans are normally faster and more predictable than vaginal birth, obstetricians are highly incentivised to deliver babies by caesarean. As a result, women may be pressured by doctors to undergo the procedure. They may also not be educated about the benefits and risks of different birthing options.
In addition, there is evidence that some women who choose vaginal birth may experience mistreatment during labour, such as neglect or physical abuse, at the hands of healthcare professionals. This is known as obstetric violence. The preference for caesarean delivery therefore comes not only from doctors, but also from women who have heard such stories and want to protect themselves.
Striking a balance between supporting all women to make informed choices while keeping caesarean rates within the optimal range is not a simple task.
Case study 3: the UK
The situation is different yet again in the UK. As a high-income country with a world-renowned health system, its maternal mortality rate is very low at 7 deaths per 100,000 live births as of 2017. The UK has a much lower caesarean rate than Brazil – 29% as of May 2020 – but still exceeds the globally accepted optimal rate.
Healthcare professionals are often pressured to make overly cautious treatment decisions to protect their professional registration – a phenomenon called defensive medicine. This has been known to affect birth workers, with high numbers of obstetricians and midwives reported to practise defensively. Practitioners may try to cover all bases and encourage women to give birth in hospitals, where they are theoretically safer because they can access emergency care and interventions if needed. The practitioner is less likely to be sued or have their professional registration revoked if something goes wrong.
For many women, the hospital is not an ideal birthing environment: bright lights, loud noises and shift changes for hospital staff are stressors that counteract the feelings of safety needed for the hormonal changes of birth to take place. In combination with the common use of epidural anaesthesia, which restricts a mother’s movement and her urge to push, the physiology of birth is compromised and a greater number of women will need obstetric interventions such as forceps or a caesarean to deliver.
What would be the ideal future for caesarean birth?
Three case studies cannot provide a comprehensive global picture of caesarean birth, but they do demonstrate the disparities in this area. We must ensure adequate provision of caesareans where needed, while managing them to prevent overuse.
Caesareans are not inherently good or bad for public health, and striking a balance between supporting all women to make informed choices while keeping caesarean rates within the optimal range is not a simple task. These case studies highlight a complex web of factors, including cultural values, health funding and women’s agency, which all feed into the caesarean rates we see.
Whether you are in Chad, Brazil, the UK or anywhere else, giving birth is no easy feat. We must help all women feel safe, supported, and in control of their bodies and choices. This will give all babies the best start to life, no matter how they come into the world.


