
What is health policy?
4 April 2024

Navigating health policy and understanding what drives policy change are essential skills for future health leaders.
A couple of years ago, I began teaching a course on health policy and practice at UCL’s new Global Business School for Health. Some of the key questions I was trying to address in the MBA class were about what health policy is and the factors that contribute to policy change over time, while also thinking of my target audience (a truly global mix of healthcare professionals, digital health experts, and other early-career professionals from around the world).
I went back to conceptual frameworks and academic readings, and dug deep into my own experience. The World Health Organization (WHO) defines health policy as ‘decisions, plans, and actions that are undertaken to achieve specific healthcare goals within a society’ (WHO, 2011). What this definition fails to convey is the breadth of what health policy covers. It is about many things, all at once:
- protecting populations from risks to their health (e.g. introducing anti-tobacco policies, hospital hygiene practices)
- strengthening health systems (e.g. investing in the health workforce or digital health policies)
- improving the prevention and care pathways for specific conditions (e.g. developing cardiovascular disease or cancer plans)
- ensuring care is equitable, responsive, accessible and of high quality (e.g. setting quality standards or accountability mechanisms for healthcare organisations).
Why does health policy matter?
Health policy is more than a composite of individual policies targeting health. It is a set of principles, ideas, rules and boundaries that provide the foundation on which individual policies are structured. Health policy has a strong cultural component – for example, around whether individuals should be given more responsibility for their health, or whether private sector involvement is a good or bad thing.
History has shown us that investing in health is a prerequisite for economic and social prosperity. This is reflected in the United Nations’ Sustainable Development Goals, of which many include components related to health. Importantly, goal 3 is devoted entirely to health and wellbeing. In 2001, economist Jeffrey Sachs coined the phrase ‘health is wealth’, showing a linear relationship between national GDP and life expectancy. The WHO Pan-European Commission on Health and Sustainable Development went on to say that ‘we can no longer accept a situation in which we fail to place sufficient value on health’ for ethical, economic and security reasons. When governments fail to invest in the health of their people, this can undermine trust in political institutions, potentially threatening democracy at its core. And this lack of trust may be felt most acutely in underserved communities, exacerbating existing inequalities.

History has shown us that investing in health is a prerequisite for economic and social prosperity. This is reflected in the United Nations’ Sustainable Development Goals, of which many include components related to health.
The need for an intersectoral approach in health policy
Improving population health is the main goal of health policies, and yet health is influenced by more than just health policies. It follows that a ‘health in all policies’ approach is needed. This means that different sectors, such as environmental or housing, consider the health implications of their policies and work together to improve population health.
At the individual level, it means recognising that a person’s health is influenced by multiple factors – the social determinants of health – and solutions need to target these root causes, and the interplay between them, to have a real impact.
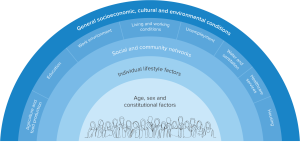
Adapted from: Dahlgren G, Whitehead M. 1991. Policies and Strategies to Promote Social Equity in Health. Stockholm, Sweden: Institute for Futures Studies.
What drives policy change?
Easy answer? It depends. Multiple models exist, but perhaps the most compelling conceptual framework is the Kingdon Streams Model, which identifies three causes of policy change: problem, policy and politics.
‘Problem’ can mean that a new issue comes to the political agenda, for example because of pressure from advocacy groups or a shift in epidemiology (e.g. a pandemic). ‘Policy’ is about a shift in process, for example a shuffling of government departments. ‘Politics’ is about political will and convergence of interests within government towards the need for change.
The confluence of these three streams creates a window of opportunity for policy change. And the key factor is time – these changes may happen concurrently, or at different times, but somehow a tipping point occurs and a change in policy is proposed.
The Kingdon Streams Model assumes a fairly rational process, though there are many who suggest that the only stream that really matters is the politics stream, and that policy change is more chaos than process.
I take a less cynical view: I strongly believe in the ability of evidence to drive policy change, and the power of advocacy to change ideas governing policy. Invariably, the most powerful driver of policy change is people – not only those with the ability to change policy, but also those who can influence it by challenging the governing values and interests and communicating a compelling, evidence-based case for change.
Who can effect change in policy?
Civic society has a strong role to play in shaping policy – think back to the role of ACT UP in shaping HIV/AIDS policy in the 1980s and 1990s. But policy change can also be strongly influenced by healthcare professionals, the general public and the private sector.
The ideal scenario is that all ‘advocates’ come together to join forces, creating a case for change that takes account of all perspectives and unmet needs. A powerful example of this is the WHO Framework Convention on Tobacco Control, which set in motion a global movement of anti-tobacco policies that have had significant impact in many countries around the world. Similarly, global policies on antimicrobial resistance (AMR) recognise that change on the ground will require collaboration between the WHO, public health, the scientific community, healthcare professionals, pharmacovigilance and the life science industry.
The most powerful driver of policy change is people – not only those with the ability to change policy, but also those who can influence it by challenging the governing values and interests and communicating a compelling, evidence-based case for change.
Where is health policy going?
In the wake of the ongoing COVID-19 pandemic, we are left with health systems in crisis across the world. Yet the challenges facing these systems – workforce shortages, a growing population of older people often living with multiple conditions, widening social inequalities, rising non-communicable diseases, the threat of AMR and other pandemics or epidemics – remain as stark and urgent as ever.
As we wrote in our 2020 think piece looking at how to create resilient health systems in light of the pandemic, we hope governments around the world will choose the path of wise investment and system strengthening, rather than of attrition and neglect, and establish a solid foundation of health policy to govern the process and drive meaningful change.
In addition to being co-founder and Managing Director of HPP, Suzanne is Visiting Lecturer and Health Executive in Residence at UCL’s Global Business School.
