
Promising advances: our submissions to Europe’s Beating Cancer Plan
11 March 2020

HPP has made submissions to the consultation on the European Commission’s beating cancer plan, focusing on three key areas.
For anyone working in the field of cancer in Europe, last week marked an exciting milestone, as the European Commission closed its first consultation on its evolving Beating Cancer Plan.
The new Commission has put cancer centre-stage, with the drafting of this ambitious plan to be launched at the end of the year, and the designation of cancer as one of its mission areas – part of the €100 billion Horizon Europe programme of investment in research.
At HPP, we’ve made several submissions to the consultation. We have focused on three areas that we believe are important considerations for the development of the EU’s and all future cancer plans:
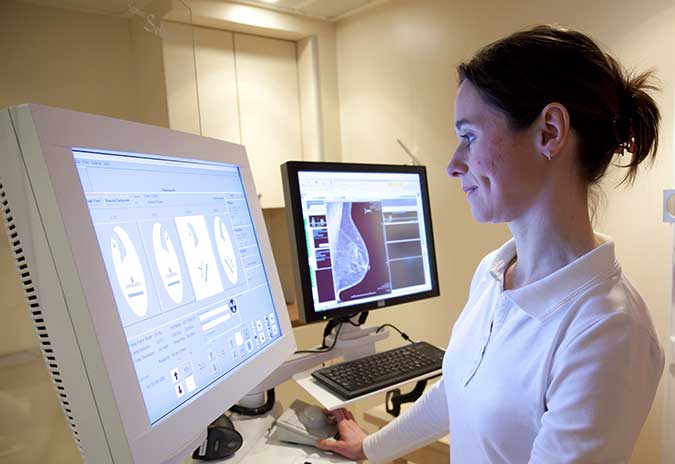
Screening programmes are available at scale only for breast, cervical and, in some countries, colorectal cancer – with varying participation rates.
Early detection
A figure often cited is that up to 20% of cancers can be prevented. This figure is somewhat misleading, however, and belies the complexity of cancer and its multiple causes. Known risk factors, such as diet or smoking, explain only a minority of cancer cases. Screening programmes are available at scale only for breast, cervical and, in some countries, colorectal cancer – with varying participation rates. Vaccinations against infections causing cancer currently exist only for hepatitis B virus (a cause of liver cancer) and human papillomavirus (HPV, a cause of cervical cancer). So there is definitely a lot of room for development in the field of prevention.
What is promising is that advances in our understanding of the genetic and biological basis of cancer have led to the development of new technologies able to detect cancer at an earlier stage – which, in turn, translates into fewer patients with advanced-stage cancers and fewer resulting deaths. For example, next-generation sequencing (NGS) techniques now make it possible to detect multiple genetic mutations at once, and tests such as liquid biopsies can identify the presence of many different cancer types with a single blood test.
The challenge, as ever, is to translate science into practice. Key questions include how these potential innovations can be used in practice, which populations they should target, and how they fit into current care pathways. It will also be crucial to train staff to communicate findings to individuals being tested (who are not yet ‘patients’). These translational challenges have been recognised in the Beating Cancer Plan Roadmap – and exciting early detection programmes, such as the Early Cancer Detection Europe (ECaDE) initiative and the International Alliance for Cancer Early Detection, are being pioneered across Europe and internationally.
Treatment encompasses far more than drugs, and all treatment options should be explored to meet the needs of each patient.
Optimising treatment for all patients
There has been much (deserved) excitement over the past decade about advances made in cancer medicine. But it is important to recognise that ‘treatment’ encompasses far more than drugs, and that all treatment options should be explored to meet the needs of each patient. This is an underlying principle behind adopting a multidisciplinary approach to care.
But this does not happen consistently enough – with a real impact on the treatments being offered to patients. For example, it has been estimated that approximately half of all cancer patients should be given radiotherapy according to clinical guidelines, yet at least a quarter of those who need it do not receive it. Reasons include shortages in high-quality equipment and trained personnel, lack of integration of those delivering radiotherapy into multidisciplinary cancer teams, and limited investment in research into radiotherapy to inform clinical practice. Negative perceptions about the use of radioactive materials may also contribute to limited access. These limitations also apply to other treatment approaches that rely on the use of radioactive materials, such as radioligand therapy (also referred to as radionuclide therapy or molecular radiotherapy).
As the treatment landscape evolves for cancer care, due consideration of these many treatment approaches – and attention to the barriers that may limit their availability to patients – is needed in future cancer plans and service delivery models.

For many people, cancer has become a chronic disease, and the need for care and support does not stop after the patient leaves the hospital.
Making integrated, multidisciplinary care a reality
An essential element of improving our response to cancer is listening to the patient perspective. HPP worked with members of All.Can on the All.Can patient survey, which found that lack of coordination or appropriate information on the far-reaching impact of cancer on patients’ lives – physically, emotionally, mentally and financially – had a deep effect on their experience of care, and their potential outcomes.
Current models of care and services do not adequately address all these needs – and a multidisciplinary approach to care is, sadly, not on offer to all patients. For many people, cancer has become a chronic disease. And as with many other chronic conditions, the need for information, care and support does not stop after the patient leaves the hospital. New models of care are required, with greater integration between hospital and community services, to ensure every person with cancer gets the care they need.
This is an exciting time in the fight against cancer, with the Beating Cancer Plan and the Horizon Europe cancer mission making ambitious strides towards reducing the burden of cancer on people, systems and societies. A careful balance will be needed to ensure that while we push for investment in exciting innovations, we never lose sight of the fundamentals, such as meeting people’s needs for information, psychological support and well-coordinated care.
Through our research at HPP, we have seen evidence of promising work in all these areas, and we are delighted to be able to contribute to international approaches to tackle this urgent healthcare issue.


