
Sharing benefits from the use of biosimilar medicines across care pathways
22 June 2022

The appropriate use of biosimilar medicines can expand treatment to more patients and create savings for health systems. These savings can then be re-invested to improve outcomes.
‘We need to break down the siloes.’ This rallying call sounds like something you’d see on a placard at a demonstration, but in fact it was the takeaway message from a webinar hosted by the Biosimilar Medicines sector group of Medicines for Europe, which I had the pleasure of moderating.
What are biosimilar medicines?
Biosimilar medicines are equivalent, though not identical, versions of biological medicines (medicines based on a biological mechanism) which have already been approved for use. Biological therapies are now the mainstay of treatment for many conditions, including cancer, inflammatory conditions (e.g. rheumatoid arthritis, psoriasis) and diabetes – but access to these treatments is often limited for financial and other reasons. As biosimilar medicines are developed after the patent of the biological medicine has expired, they are usually a less expensive alternative, offering physicians a better-value, but equally effective, option to treat their patients.
Biosimilar medicines can drive more efficient care
Many countries have advocated for appropriate use of biosimilar medicines as an important way of driving more efficient care. The possible financial savings are enormous: with over 100 medicines opening up for biosimilar competition between now and 2030, €286 billion could be saved. It goes without saying, however, that – as for all therapeutic interventions – the choice of a biosimilar medicine must be guided by what is best for each individual patient.
The possible financial savings are enormous: with over 100 medicines opening up for biosimilar competition between now and 2030, 286 billion Euros could be saved.
How can biosimilar medicines improve care?
The benefits of using biosimilar medicines are not merely financial: they may also make early treatment available to more people. For example, in inflammatory bowel disease (IBD) early intervention with biological medicines is associated with improved outcomes – yet studies in Italy show that over one in four people with IBD eligible for biological therapy do not receive it. The Italian gastroenterology clinical community has worked together to ensure appropriate biosimilar policies were integrated into clinical guidelines, and in several academic medical centres these policies have allowed more people to start treatment earlier, with better outcomes.
Re-investing savings into other areas of healthcare
Benefits do not only extend to medicines – and this was the key topic of the webinar. The savings made by using biosimilar medicines can be re-invested into other aspects of care, benefiting a broader population.
This ‘beyond medicines’ approach has been recognised by the largest national health insurance fund in France, Caisse Nationale d’Assurance Maladie (CNAM), which created a special article of law allowing local healthcare settings to re-invest savings incurred from using biosimilar medicines into system improvements. Local providers (physicians, hospitals, pharmacists) are given the freedom to determine how to re-allocate resources in their local setting (such as the hospital they practise in). A core goal of the project is to break down traditional siloes in funding streams between the hospital and community settings, medication budgets and other budgets, encouraging all clinical teams to work towards a common goal.
Another powerful example is in Cardiff, Wales. People with lymphoma were offered the choice of a biological therapy, which had a much shorter injection time, or its biosimilar equivalent, which had longer administration time but was less costly to the clinic. The clinic consulted with patients on what would be best for them, and discovered that the potential benefits of a shorter infusion time were offset for the patients by the time they needed to travel across town to reach the clinic. A decision was therefore taken to re-invest the financial savings from using biosimilar medicines to staff new infusion clinics close to people’s homes in the outskirts of the city. This approach created shared benefits for patients and the clinic.
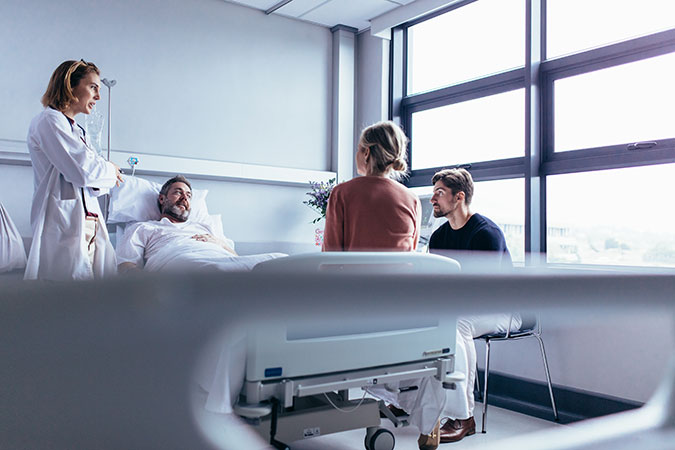
These solutions take a truly person-centred approach: decisions as to how best to allocate savings are made in close consultation with the people receiving care, and focus on what will make the most difference to them.
Implementing a multidisciplinary, person-centred and whole-system approach
It is important to underline how innovative these approaches are. First, they take a whole-system approach to driving efficiency in care – something that has long been advocated by the likes of All.Can. Second, and most important, they take a truly person-centred approach: decisions as to how best to allocate savings are made in close consultation with the people receiving care, and focus on what will make the most difference to them.
What was also fascinating about this webinar – and frankly, so refreshing – was that all panellists came to the same conclusion from very different professional perspectives. Panellists included a representative from a biosimilar medicine company; a public health professional; a health insurer; a practising physician; and me – a policy researcher. This multi-sectoral and multidisciplinary thinking is needed to determine what policy measures can enable such forward-looking re-investment opportunities.
The question we were left with at the end of the webinar is how to scale up this approach. The benefits of multiplying initiatives such as those presented here would be considerable, particularly in the management of non-communicable diseases (NCDs). Disparities in access to all aspects of NCD prevention and care are a recognised challenge in many countries, and risk being exacerbated with growing economic pressures on health systems recovering from the COVID-19 pandemic.
As was demonstrated during the webinar, we all need to work together, using flexibility and creativity, to find ways of using resources as effectively and efficiently as possible, never losing sight of our ultimate goal of improving outcomes for everyone. Maybe breaking down the siloes should be our rallying call after all.
For further perspectives from the webinar, see this blog by Medicines for Europe.


